
|
|||||||
Chondromalacia Patellae
What is Chondromalacia patellae?
Chondromalacia literally means "softening of the cartilage", and Patellae means "the knee-cap". So Chondromalacia patellae means "softening of the articular cartilage of the knee-cap." The articular cartilage is the cartilage lining under the knee-cap that articulates with the knee joint. Under normal circumstances, it is smooth and shiny, so that it glides smoothly along the articular groove of the femur as the knee bends. When it "softens", it may break down, causing irregularities along the undersurface of the patella.
What causes Chondromalacia patellae?
Chondromalacia patellae occurs in two distinct age-groups:
- It can happen in the older age-group (in the 40’s and beyond) when the articular cartilage breaks down as part of the wear-and-tear process that occurs with the rest of the body. The patella cartilage is one of the earliest places where cartilage breakdown occurs, and is slowly progressive, leading to degenerative arthritis (osteoarthritis) in the knee joint.
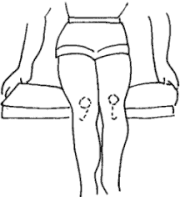
- It can occur frequently in teenagers (especially girls) when the articular cartilage "softens" in response to excessive and uneven pressure on the cartilage, due to structural changes in the legs with rapid growth, and muscle imbalance around the knee. During periods of rapid growth, especially in girls, any knee valgus (knock-knees) is accentuated, thereby increasing the Q-angle, the angle formed by the thigh and the patellar tendon (see diagram). Any flexion of the knee increases the tendency of the patella to dislocate. Undue pressure is placed on the lateral (outer) facet of the patella. Moreover, in many of these teenagers, the vastus lateralis and vastus medialis components of the Quadriceps muscle are not well-balanced. The vastus lateralis tends to be more powerful than the vastus medialis, thus increasing the tendency for the patella to track or dislocate laterally. This again puts undue pressure on the lateral facet. This uneven and excessive pressure on the lateral facet of the patella leads to cartilage "softening" and breakdown.
What are the symptoms?
The typical patient is a teenage girl complaining of pain in the front of her knee around the knee-cap. She may also have pain that is deep-seated that may radiate to the back of the knee. The pain comes and goes, but usually with squatting, kneeling, and negotiating steps, especially going down the stairs. She may be engaged in strenuous sports, but experiences pain with repeated bending of the knees. Although girls are more often affected, boys can have this problem too.
At this stage, there is no breakdown of the articular cartilage of the patella yet, and is totally reversible. In fact, many doctors may not use the term "chondromalacia patellae" at this stage, because there is no actual softening or breakdown of the cartilage. A more appropriate diagnosis would be "Anterior knee pain syndrome" or "Patellofemoral stress syndrome". In fact, in the majority of patients, the pain comes and goes for a few years until growth is complete. At that point, the pain goes away permanently. In others, the pain gets increasingly worse during the teenage years, the articular cartilage of the patella may actually break down, and medical or surgical treatment may be necessary.
How do you prevent it?
In a sense, whether a child will develop this problem of anterior knee pain and chondromalacia patellae depends on the morphology of the knee and any muscle imbalance she may have. If she is lanky and knock-kneed, she is more likely to develop the condition. If she has tightness of her lateral muscles, she may be more prone to the problem.
Regardless of the above, the best way to minimize the chances of developing chondromalacia patellae is to warm-up and stretch out before sports, especially your quadriceps and hamstrings. If possible, vary your sports. For example, alternate running with swimming with bicycling. Avoid squatting, kneeling, stairs and hill running if you can. In addition there are some exercises that are helpful in preventing and helping the symptoms of anterior knee pain. These exercises should be done regularly, twice a day. If symptoms are already present, it will take about 6 weeks before you get the benefit of the exercise. So, the key is to be consistent, and persistent.
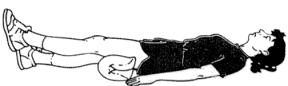
Short-arc extensions are done sitting up or lying down. Use a
rolled-up towel to support your thigh while you keep your leg and foot
in the air for 5 seconds. Lower your foot as you bend your knee slowly.
Repeat 10 times for each leg, twice a day.
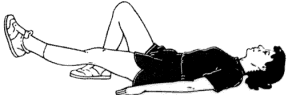 Straight-leg
raises are done lying down. Lift your whole lower limb at the hip
with the knee extended, and keep it up in the air for 5 seconds. Then
lower slowly. Repeat 10 times for each leg, twice a day.
Straight-leg
raises are done lying down. Lift your whole lower limb at the hip
with the knee extended, and keep it up in the air for 5 seconds. Then
lower slowly. Repeat 10 times for each leg, twice a day.
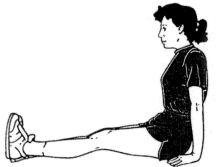 Quadriceps isometric exercises are done sitting up, with your legs
extended in front of you. Tighten your quadriceps muscles by pushing the
knees down onto the floor. Hold for 5 seconds. Repeat 10 times each leg,
twice a day.
Quadriceps isometric exercises are done sitting up, with your legs
extended in front of you. Tighten your quadriceps muscles by pushing the
knees down onto the floor. Hold for 5 seconds. Repeat 10 times each leg,
twice a day.
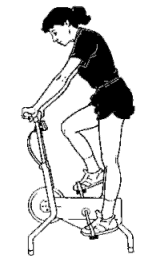 Stationary
bicycling on low tension setting improves your exercise tolerance
without stressing your knee. Adjust your seat high enough so that your
leg is straight on the down stroke. Start with 15 minutes a day and work
up to 30 minutes a day.
Stationary
bicycling on low tension setting improves your exercise tolerance
without stressing your knee. Adjust your seat high enough so that your
leg is straight on the down stroke. Start with 15 minutes a day and work
up to 30 minutes a day.
What does your doctor do about it?
After taking a history and performing a physical examination, your doctor may order an X-ray of the knee. In most instances the X-rays are normal, but it is still important to rule out any other significant problems. The patella view or "sunrise" view may show the patella is displaced or tilted laterally, a confirmation that the vastus lateralis muscle is over-powering or too tight.
For the teenager with chondromalacia, the objective of treatment is to restore normal patella alignment with the help of exercises. The only way to alter knee morphology is by performing surgery, and sometimes that is required. However, in most cases, exercises with or without formal physical therapy is all that is needed to correct the problem. The exercises described above concentrates on strengthening the vastus medialis obliquus (VMO), responsible for stabilizing the patella. Once that strengthens, and muscle balance is restored, the pain improves. In some cases, if the pain persists, your physician may prescribe physical therapy. The therapist will work at stretching the vastus lateralis, as well as strengthening the Quadriceps muscle and Hamstring muscles, using manual and electrical techniques. Occasionally the therapist may employ a technique called "patella taping" to keep the patella from tracking laterally.
A non-steroidal anti-inflammatory medication like Motrin is often prescribed by your physician. This is taken regularly, whether you feel pain or not. By decreasing the inflammation, the pain is often reduced. But not only that, there is some evidence to suggest that the drug actually helps in reforming the articular cartilage.
A knee brace is also often prescribed for patients who want to stay active in sports. The usual brace prescribed is what is known as a patella stabilizing brace. It consists of a knee sleeve with a patella cutout, and a horse-shoe pad based laterally to keep the patella from tracking laterally. (see the AirPro™ Patella Knee Support)
With conservative treatment, about 85% of patients improve enough that no further treatment is needed. In about 15% of patients, the pain stays severe, or becomes worse that surgical treatment is needed.
An MRI exam is usually not indicated for most cases of chondromalacia, unless the doctor suspects any other pathology.
The form of surgery done is usually an arthroscopic surgery. The surgery is performed through little keyhole incisions with the help of an arthroscope. It is usually performed as an outpatient procedure, under a light general anesthetic. The surgeon will check out the knee through the arthroscope, and confirms the lateral patella tracking. To correct the problem, a lateral release, consisting of dividing the vastus lateralis muscle is performed. This is done from the interior of the knee, so there is no visible incision from the outside. By dividing the vastus lateralis, this muscle is weakened, and if tight, stretched out; hence restoring balance to the Quadriceps muscle. Post-operatively, Physical therapy for 6 weeks will restore the knee back to health, and the patient back to sports.
In some patients, the pain continues even after surgery and intensive physical therapy. This happens especially in patients with severe structural problems, like markedly increased Q-angle and lateral subluxation or dislocation of the patella. When that happens, more than a lateral release is required. Open surgery is occasionally done for the recalcitrant case, and usually involve extensive open realignment of the Quadriceps mechanism and even bone work to correct the problem.
What can be expected after treatment?
Most patients do well with treatment. It is important that you keep up with the Quadriceps exercises on an indefinite basis. It takes only 5 minutes twice a day, and is a worthwhile long-term investment for your knees. Also, make sure you stretch adequately and warm up before sports.
NOTICE: The information presented is for your information only, and not a substitute for the medical advice of a qualified physician. Neither the author nor the publisher will be responsible for any harm or injury resulting from interpretations of the materials in this article.
Questions
or comments? Post your thoughts in the Orthoseek
Message Forum!
Find a pediatric orthopedic surgeon
in an area near you.
Home | About Us | Orthopaedic Topics | Message Forum
![]()
Comments, questions, or suggestions are welcome. Please
contact us using this form.