
|
|||||||
Spondylolysis and Spondylolisthesis
What is it?
The spine or vertebral column consists of a series of vertebrae held together to give support for the spinal cord and nerves arising from it. Each vertebra consists of an anterior vertebral body, and a posterior bony ring with two superior facets and two inferior facets that articulate with the neighboring vertebrae. These articulations form the posterior facet joints that provide stability to the spine.
In spondylolysis, there is a defect in the pars interarticularis (which literally means the "piece between the articulations"). So spondylolysis means a defect in the thin isthmus of bone connecting the superior and inferior facets, and could be unilateral (involving one side) or bilateral (involving both sides). Although the defect can be found at any level, the commonest vertebra involved is the 5th Lumbar vertebra (or L5).
In cases of bilateral spondylolysis, the posterior articulations can no longer provide the posterior stability, and anterior slipping of the L5 vertebra over the sacrum could result. This slip is called Spondylolisthesis.
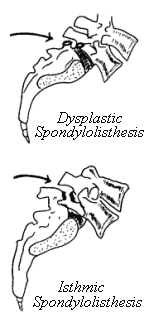
Spondylolysis is the commonest cause of spondylolisthesis, and is sometimes referred to as isthmic spondylolisthesis, since the defect is in the isthmus. But there are other causes of spondylolisthesis. In children born with underdeveloped facet joints (dysplastic joints), spondylolisthesis can also result, and is sometimes referred to as dysplastic spondylolisthesis. More rarely, any infection or tumor affecting the posterior bony ring including the facet joints, can also cause instability and spondylolisthesis.
What causes it?
The commonest cause of spondylolisthesis is spondylolysis, and it is the cause of spondylolysis that is the subject of intense debate.
Some people feel that it is an inherited defect of the pars interarticularis. In surveys of asymptomatic school children, spondylolysis is present in 4 to 6%. In certain racial groups like the Eskimos, the incidence is as high as 40%, suggesting a genetic factor. Spondylolysis has been reported in an infant, although it is rare before age 4.
However, certain other observations point to a repetitive trauma etiology. Incidence goes up with age, and incidence is higher in children involved in certain kinds of sports like gymnastics, weight-lifting and football that put a lot of stress on the back. In gymnastics, the hyperextension position of the lumbar spine places excessive stress on the back, leading to stress fractures in the pars interarticularis.
In an attempt to unify the two etiological theories, most physicians believe that most children with spondylolysis may be born with a "weak" pars interarticularis. Repeated stress with activities during the years of growth between 8 and 14 causes the "stress fracture" that leads on the spondylolysis.
What are the symptoms?
Most children with spondylolysis, and even some children with spondylolisthesis are aymptomatic, and may grow up not even aware that they have the conditioin.
For those with symptoms, back pain is probably the most common symptom, and presents during the adolescent growth spurt. There is often a history of trauma at sports, usually trivial, and an X-ray reveals the "fracture". If the child continues to have good range of motion of the back, it is probably safe to say that the spondylolysis is not due to that particular injury, but a result of years of cumulative stress of the back.
Sometimes the child is brought in by the parents because of poor posture or funny gait. This is usually due to spondylolisthesis, causing muscle spasm in the back that makes the back stiff, and tight hamstrings causing the child to walk with the knees bent, and a short stride. Sometimes, there is an associated scoliosis that is more obvious to the observer than the spondylolisthesis.
How do you prevent it?
There is not too much you can do about your genes, but there is certainly something you can do about your activities. Avoiding sports in the growing years is usually not an option, but you can choose your sports wisely. For your little gymnast, limiting the number of hours of practice (unless she is an aspiring Olympian), or alternating gymnastics with another sport like swimming or bicycling may be helpful. There is no place for weight-lifting in the pre-pubertal child.
If your child was incidentally found to have spondylolysis with no symptoms, there is no need to restrict his or her activities. The chances of an aymptomatic spondylolysis developing a slip is not high enough to justify restriction of activities.
What does your doctor do about it?
If your child presents with any of the symptoms described earlier, you doctor will order an X-ray of the lumbo-sacral spine to rule out spondylolysis. Very often, the oblique views are best for revealing the defects in the pars interarticularis. If there is spondylolisthesis or slip, the lateral view will show it best.
If your child has spondylolysis, treatment is directed towards reducing the backpain by use of anti-inflammatory medications like Ibuprofen, and stretching and strengthening exercises for the back and abdominal muscles. In more severe cases, a lumbosacral support and Physical therapy may be ordered. After 1 to 2 weeks of rest, the pain usually goes away, and the child may resume sports.
In the most severe cases where there is severe trauma and muscle spasm, a nuclear bone scan may be done to check if the pars defect is indeed a fracture. If so, it may be necessary to place the child in a rigid lumbosacral orthosis or even a body cast. Sports will be curtailed for 3 months to allow time for healing.
In patients with spondylolisthesis, the treatment depends on several factors, depending on age, sex, and severity of slip. The younger child has a higher chance of further slip with growth. Girls are more prone to progressive slip than boys. Severity of slip is estimated on the lateral view on X-ray, and depends on the amount of contact left between the L5 and S1 vertebral bodies. Grade 1 indicates more than 75% of contact. Grade 2 indicates 50 to 75% of contact. Grade 3 indicates 25 to 50% of contact. Grade 4 indicates less than 25% of contact. The higher the grade of slip, the more serious the problem, and the higher the chances of further slip.
A CT scan or even an MRI may sometimes be needed to further elucidate the bone and nerve problem before treatment is started.
For Grades 1 and 2, conservative treatment is usually instituted. This will be similar to treatment for spondylolysis, except for use of a rigid Lumbosacral orthosis LSO or thermoplastic brace), and intensive physical therapy to strengthen the back and abdominal muscles, as well as stretching exercises for the tight hamstring muscles. X-rays (lateral views only) are done every 3 to 6 months to check on the severity of the slip. If the patient responds to conservative treatment, the pain resolves, the hamstring tightness improves, and the patient may return to limited sports. Gymnastics, weight-lifting and football should be avoided. If the pain does not improve, or if follow-up X-rays demonstrate further slip, surgery may be needed.
Surgery consists of fusing the L5 to the S1 vertebrae to prevent further slipping. Depending on the degree of slip and other factors, your surgeon may fuse the vertebrae "as is", or fuse the vertebrae after attempting to reduce the slip. This latter technique entails significant risk to the spinal nerves, and will have to be taken into consideration in the pre-operative planning.
What can be expected after treatment?
If your child has spondylolysis discovered incidentally, and has no symptoms at all, there is no need to restrict his or her activities. As long as he or she has no symptoms, no regular follow-up is needed.
If your child has spondylolysis discovered because of back pain, and he or she responds to treatment, there is no need to restrict activities as long as there is no pain. The chances of this developing into spondylolisthesis is indeed very small, with or without participation in sports.
If your child has spondylolisthesis (slip), care needs to be exercised, especially in girls of young age. Up to the age of 14 or 15, the risk of further slip is the highest, and regular follow-up is needed. Sports participation is allowed, but strenuous sports like gymnastics, weight-lifting and football should be avoided.
If surgery is needed, spine fusion is the procedure most often done, and results tend to be good.
NOTICE: The information presented is for your information only, and not a substitute for the medical advice of a qualified physician. Neither the author nor the publisher will be responsible for any harm or injury resulting from interpretations of the materials in this article.
Questions
or comments? Post your thoughts in the Orthoseek
Message Forum!
Find a pediatric orthopedic surgeon
in an area near you.
Home | About Us | Orthopaedic Topics | Message Forum
![]()
Comments, questions, or suggestions are welcome. Please
contact us using this form.