
|
|||||||
Clubfoot
 What is clubfoot?
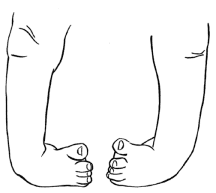
What is clubfoot?
Clubfoot is a congenital deformity of the foot that occurs once per 1000 live births in the U.S. The foot has a typical appearance of pointing downwards and twisted inwards. Since the condition starts in the first trimester of pregnancy, the deformity is quite established at birth, and is often very rigid.
What causes clubfoot?
No one really knows what causes the deformity. It tends to be more common in boys, although girls are not exempt. There may be a positive family history. In rare instances a child born with myelomeningocele (spina bifida) or arthrogryposis may also have clubfeet. Beyond these observations, no actual cause is known. If your child has clubfoot, it is usually not due to anything you did or did not do during pregnancy.
During development, the posterior and medial tendons and ligaments (in the back and inside) of the foot fail to keep pace with the development of the rest of the foot. As a result, these tendons and ligaments tether the posterior and medial parts of the foot down, causing the foot to point downwards and the twist inwards. The bones of the feet are therefore held in that abnormal position. Over time, if uncorrected, the bones will become mis-shapened.
What are the symptoms of clubfoot?
Clubfoot does not cause pain in the infant. Because it is so obvious, it is usually discovered at birth. If left untreated, the deformity does not go away. It gets worse over time, with secondary bony changes developing over years. An uncorrected clubfoot in the older child or adult is very unsightly, and worse, very crippling. The patient walks on the outside of his foot which is not meant for weight-bearing. The skin breaks down, and develops chronic ulceration and infection.
What does your doctor do about it?
Treatment should be started right away. The initial treatment consists of manipulating the foot to get it to the best position possible, and then holding the correction in a cast. The cast is changed on a weekly basis, with manipulation before each casting, to obtain further correction. After the first 6 weeks, the foot is manipulated and casted every 2 weeks.
In 50% of cases, manipulation and casting is successful, and the foot can then be placed in a thermoplastic brace to hold the correction. In 50% of cases, manipulation and castings alone do not correct the deformity completely. At that point somewhere between 3 to 6 months, a decision will be made regarding further castings, or surgery.
Some surgeons prefer to wait till the child is about 1 year old before performing surgery, to allow the foot to get a little larger to facilitate surgery. Other surgeons operate as early as 3 months of age if it was clear that further castings will not achieve any more correction. Your surgeon will have to make that decision with you individually.
Surgery consists of releasing all the tight tendons and ligaments in
the posterior and medial aspects of the foot, and repairing them in the
lengthened position. More recently, it has been recognized that some of
the lateral ligaments have to be released as well, to allow a complete
release. The incision used may vary. Many surgeons prefer to make two
separate incisions, a posteromedial incision, and a small lateral incision
for the lateral structures. Other surgeons prefer to make a circumferential
incision encompassing the heel and both medial and lateral aspects of
the foot. Either technique does an adequate job, with its attendant pros
and cons. A surgeon normally uses the technique he is comfortable with.
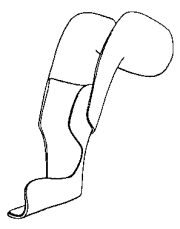
After surgery, the foot needs to be casted at biweekly intervals for
6 weeks, followed by the use of a thermoplastic brace, e.g., Wheaton
Brace, to hold the correction. The brace is used full-time for about
6 weeks, followed by night use only till the child starts to walk at one
year of age.
What can be expected after treatment?
Up to the age of one year, there is a 25% chance of recurrence after surgical correction. Close follow-up is therefore needed. By age one, if the foot stays well corrected, standing and walking lessens the chance of recurrence, and the foot usually stays corrected.
The objective of clubfoot treatment is to obtain a plantigrade and flexible foot. "Plantigrade" means the child stands with the sole of the foot on the ground, not on his heels or the outside of his foot. "Flexible" means one can move the foot around freely without pain.
When recurrence occurs, further surgery is needed. In the younger child, soft tissue releases and lengthenings may suffice. In the older child, because of bone changes, surgery involving osteotomy (cutting the bone) is usually needed.
Clubfoot surgery is difficult, and requires meticulous attention to details. Even in the best of hands, failures and recurrences can occur. It is therefore important that the surgery be done by a surgeon experienced in working with children’s feet.
NOTICE: The information presented is for your information only, and not a substitute for the medical advice of a qualified physician. Neither the author nor the publisher will be responsible for any harm or injury resulting from interpretations of the materials in this article.
Questions
or comments? Post your thoughts in the Orthoseek
Message Forum!
Find a pediatric orthopedic surgeon
in an area near you.
Home | About Us | Orthopaedic Topics | Message Forum
![]()
Comments, questions, or suggestions are welcome. Please
contact us using this form.