
|
|||||||
Carpal Tunnel Syndrome
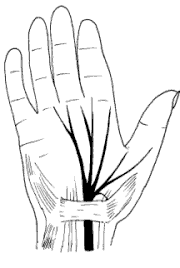
What is carpal tunnel syndrome (CTS)?
Carpal tunnel syndrome is a condition where the median nerve at the wrist is being compressed, causing pain and numbness in the hand. The median nerve is a major nerve that supplies sensation to the hand. It runs within a tunnel called the carpal tunnel at the wrist. The carpal tunnel is made up of the carpal bones forming its base and sides, and a thick band of fibrous tissue called the flexor retinaculum forming its roof. Structures that run within the carpal tunnel include the median nerve and the flexor tendons to the hand and fingers.
What causes carpal tunnel syndrome (CTS)?
Any condition that causes swelling of the contents or surrounding structures of the carpal tunnel syndrome can cause carpal tunnel syndrome. This is because the carpal tunnel is an enclosed space, and any swelling encroaches on the space, thus putting excessive pressure on the median nerve. For example, a fracture of any bone at the wrist causes swelling of the tendons and ligaments at the carpal tunnel, which compresses the median nerve. In Rheumatoid arthritis, the swelling of the flexor tendons within the carpal tunnel compresses the median nerve, and can cause CTS.. During pregnancy, with water retention in the body as well as within the carpal tunnel, the median nerve is frequently compressed, causing CTS. That is why some women experience tingling in the hands just before their periods. More recently, attention has been drawn to the fact the CTS is a Repetitive Trauma Disorder (RTD). Workers who use their wrists and hands repetitively during the course of their employment are prone to CTS. Examples of jobs prone to CTS include typists, meat-cutters and mechanics. The repetitive motion of the wrist stresses the tissues at the wrist to the point where microtrauma (injury so minute that it can only be seen on the microscope) occurs. This in turn causes swelling at the carpal tunnel. If the areas of microtrauma are multiplied over a repetitive basis over weeks and months, it can lead to a full-blown CTS.
What are the symptoms?
The patient typically feels tingling and pain in the thumb, index and middle fingers. In the early stages it comes on during the night while the patient is asleep. This wakes the patient up from his or her sleep. The patient learns that by shaking his or her hands and wrists, the symptoms improve. In other instances, the patient may feel the pain and tingling while at work at the keyboard or while using a wrench or power-tool. Later on, the pain and tingling persists all the time. In the later stages, the pain and tingling may disappear, and the patient has persistent numbness in his or her hand. This is not a good sign, because it may signify nerve damage. Over time, the nerve damage may become permanent, leading to a weak grip and total loss of feeling in the hand.
How do you prevent it?
Workers in high-risk jobs that require repetitive and continuous motion of the wrist can minimize the risk of developing CTS by paying attention to the following.
- Keep the wrist in the straight or "neutral" position as much as possible. For example, if you work at a keyboard, adjust the height of your chair and desk such that your elbow and wrist are level, thus allowing your wrist to be in the "neutral" position while typing.
- When doing work involving repetitive motion of the wrists, take frequent breaks or rotate your job.
- When using tools, make sure the handle fits your hand, and you can grasp the tool with your whole hand, rather than grasping with the tips of your fingers or thumbs.
- Wear gloves whenever possible, especially when using power or vibratory tools, to avoid direct pressure on the median nerve at the wrist.
- Use good posture at work. For example, always face your task at hand squarely, so that your trunk or neck is not in the twisted position when your work. When at a keyboard, make sure that your chair has a back support so that you can sit upright, and that your chair and desk are at the right height.
- Exercise your wrists and hands regularly at work. Take a one minute break every 20 minutes to perform some of the exercises shown below.
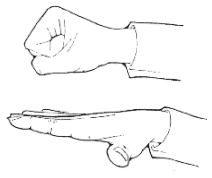
Range-of-motion exercises - Clench fist tightly for 5 seconds,
then release, straightening your fingers all the way and keep them straight
for 5 seconds. Repeat 5 times for each hand.
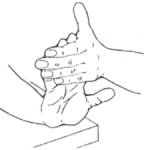
Stretching exercises - Using one hand, bend the fingers of the other hand gently as far as you can, stretching the fingers and wrist. Hold for 5 seconds. Repeat 5 times for each hand.
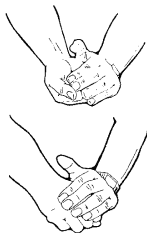
Isometric exercises - Clench fist with palm facing up. Use other hand to push down on fist, while providing resistance with the fist. Hold for 5 seconds. Repeat with palm of clenched fist facing down. Repeat 5 times for each hand.
What does your doctor do about CTS?
After an initial history and physical examination, he may order the following tests.
X-rays of the wrist may show arthritis or other bony pathology that is impinging against the median nerve at the wrist.
Electromyography and nerve conduction studies (EMG) is a test of the electrical activity in the nerves and muscles. In cases of CTS, with compression of the median nerve, the velocity of electrical conduction of the nerve may be impaired, and this is often diagnostic of the condition. In more advanced cases, there may be muscle damage, causing changes in the electrical activity in the muscles that may be detected by EMG.
MRI can confirm CTS by showing median nerve compression at the wrist. However, it is an expensive test, and often not necessary to make the diagnosis.
Treatment is usually conservative, and consists of the following:
- Non-steroidal anti-inflammatory drugs like Aspirin or Motrin can decrease swelling and fluid retention in the carpal tunnel, thus reducing compression on the median nerve.
- Use of a wrist splint whenever possible to keep the wrists at the neutral position.
- Exercises as described above.
- Instructions regarding prevention as outlined above.
In some cases, conservative treatment is not successful. Surgery is then needed. Surgery is a straight-forward outpatient procedure, which can be done under regional anesthesia.
The usual procedure involves making an incision along the skin crease next to the wrist, dividing the thick flexor retinaculum, and freeing the median nerve. The skin is then sutured together, and a bulky dressing applied.
A newer technique using a small keyhole incision and dividing the flexor retinaculum with the help of an arthroscope is sometimes used. The advantage is a smaller incision. The disadvantage is inability to visualize the median nerve at the time of surgery, so it is not indicated in all cases. Moreover, the long term results are still not known, since this is a relatively new procedure.
For the first one to two weeks after surgery, follow the doctor’s instructions closely with regard to dressing care and elevation.
Whether the surgery is done by open or closed technique, the incision usually heals very nicely. Post-operative exercises are started about two weeks after surgery, and consist of the exercises described above.
Complications can happen with any kind of surgery. In addition to complications related to anesthesia, there could be occasional instances of excessive bleeding, infection, and nerve or tendon damage, persistent weakness or numbness. Most patients however can expect to undergo surgery without any complications.
What can be expected after surgery?
Results with surgery tend to be excellent. Most of the tingling and pain disappears within two weeks. Recurrence is not frequent, especially if the patient maintains good health habits and does his or her exercises regularly.
Most office workers return to work after two to three weeks. If you do heavy work or use heavy equipment, it may take six to eight weeks. Your doctor will be able to advise you on your individual needs and requirements.
NOTICE: The information presented is for your information only, and not a substitute for the medical advice of a qualified physician. Neither the author nor the publisher will be responsible for any harm or injury resulting from interpretations of the materials in this article.
Questions
or comments? Post your thoughts in the Orthoseek
Message Forum!
Find a pediatric orthopedic surgeon
in an area near you.
Home | About Us | Orthopaedic Topics | Message Forum
![]()
Comments, questions, or suggestions are welcome. Please
contact us using this form.